If you’ve ever thought acne was a thing of the past, left behind in your teenage years, only to find yourself still grappling with breakouts well into adulthood, you’re not alone. According to the American Academy of Dermatology, acne isn’t just a phase of adolescence; adults, especially women, can experience it too.
Hormonal acne is a common issue among women after puberty, particularly in adulthood. It often flares up just before, during, or after menstrual periods in a predictable pattern. Unlike typical acne, hormonal acne tends to manifest as deeper nodules and cysts, lingering for extended periods. This type of acne is often linked to excessive sebum production, which clogs pores and leads to pimples. Typically, hormonal acne appears as spots along the chin and jawline, as well as around the mouth, and it can also affect the entire face and back. Though managing hormonal acne can be challenging, there are treatments available to help prevent future breakouts.
If you’re 25 or older and noticing pimples, whiteheads, or blackheads, you’re part of a growing number of adults, especially women, dealing with breakouts. Navigating the multitude of acne products available online and in stores can be overwhelming, making it difficult to determine which lotion, wash, or wipe will effectively clear your skin.
Acne isn’t just a concern for young teens going through puberty; it can also affect adults of any age. Approximately 40% to 50% of the adult population aged 20 to 40 years old experiences some form of acne.
While hormonal acne can affect individuals of any gender in adulthood, it’s more prevalent in women than men. Studies have revealed that around 50% of women aged 20-29 deal with acne, and 25% of women aged 40-49 also experience it. Why do women experience hormonal acne more frequently than men?
Women tend to undergo more frequent hormone fluctuations due to puberty, menstrual cycles, pregnancy, and menopause. If you’re struggling with hormonal acne, explore this guide to learn more about its causes and management strategies.
What is hormonal acne, exactly?
First, it’s essential to discern between hormonal acne and good old-fashioned pimples. Hormonal acne, also referred to as adult-onset acne, occurs when individuals aged 20 to 50 experience acne development, encompassing pimples, blackheads, whiteheads, cysts, and other forms. This type of acne is associated with hormonal fluctuations, resulting in “cyclical breakouts” that often coincide with the menstrual cycle. However, these hormonal shifts may also occur during significant life events, such as menopause or postpartum, contributing to breakouts.
It’s worth noting that hormonal acne is not an official medical diagnosis. Nevertheless, when individuals consistently experience specific breakout patterns around their menstrual cycle or during periods of significant hormonal changes, such as those associated with conditions like polycystic ovary syndrome (PCOS), dermatologists commonly classify it as hormonal acne.
What causes hormonal acne?
Hormonal acne arises from fluctuations in hormone levels, particularly estrogen, progesterone, and testosterone. These hormonal shifts commonly occur during menstruation cycles, pregnancy, and menopause, triggering the emergence of zits and pimples.
Heightened hormone levels prompt increased production of sebum, an oily, waxy substance, which subsequently instigates inflammation, alters skin cell activity, and facilitates bacterial colonization in hair follicles. This convergence of factors sets the stage for the development of acne. Additionally, hormonal acne can be influenced by medications, antibiotics, certain dietary choices, as well as psychological factors such as depression, anxiety, and stress.
Hormones Regulating Sebum
Let’s explore the details of the hormones affecting your skin. Specifically, we’re referring to sex hormones that regulate sebum production, the oil produced by your skin’s sebaceous glands. The hormones primarily responsible for regulating sebum production are:
Estrogens
Estradiol, a type of estrogen, exerts an inhibitory influence on sebum production by dampening the activity of the sebaceous glands. Nonetheless, estrogen levels vary across the menstrual cycle, affecting sebum secretion correspondingly. Notably, estrogen is pivotal in regulating and mitigating sebum production, preventing pore blockage and acne formation. However, during certain life stages like menstruation or perimenopause, estrogen levels naturally diminish.
Progesterone
Conversely, progesterone, elevated during pregnancy and ovulation, has the potential to trigger sebum secretion, potentially exacerbating skin concerns. While progesterone’s impact on sebum production is not as comprehensively understood as that of androgens and estrogens, it remains a notable factor. Progesterone levels surge in the latter half of the menstrual cycle and during pregnancy, potentially influencing fluctuations in sebum production during these periods.
Androgens
Androgens, notably testosterone, can activate sebaceous glands, fostering an environment favorable for acne-causing bacteria like Cutibacterium acnes to thrive. This explains why acne frequently manifests as a symptom of conditions such as PCOS, which involve imbalances in androgens.
Androgens comprise a group of hormones encompassing testosterone and dihydrotestosterone (DHT). They play a pivotal role in stimulating sebaceous glands to produce sebum. Testosterone, particularly influential during puberty, significantly boosts sebum secretion. DHT, a derivative of testosterone, is even more potent in stimulating sebum production.
Causes of hormonal acne within your control
- Stress
- Lack of sleep
- Use of hair and skin care products containing pore-clogging ingredients or lacking oil-free formulations (non-comedogenic or non-acnegenic)
Causes of hormonal acne beyond your control
- Fluctuating hormone levels in women, such as those occurring around menstruation, irregular periods, pregnancy, menopause, or after discontinuing birth control
- Men undergoing testosterone treatment
- Family history of acne (genetic predisposition)
- Side effects of medications (such as steroids)
- Pre-existing medical conditions (such as polycystic ovary syndrome, other ovarian conditions, and metabolic conditions)
Biotin and Acne
It’s important to be aware of the potential link between biotin supplements and acne breakouts. While biotin is often taken for hair and nail health, there is a misconception that it causes acne. For more detailed information, read our post on Debunking the Biotin-Acne Myth.
Retinol Skin Purging
When introducing retinol into your skincare routine, you might experience what is known as skin purging. This is a common reaction where your skin temporarily breaks out before it gets better. To understand more about retinol skin purging, check out our blog post on Is Your Skin Purging From Retinol?.
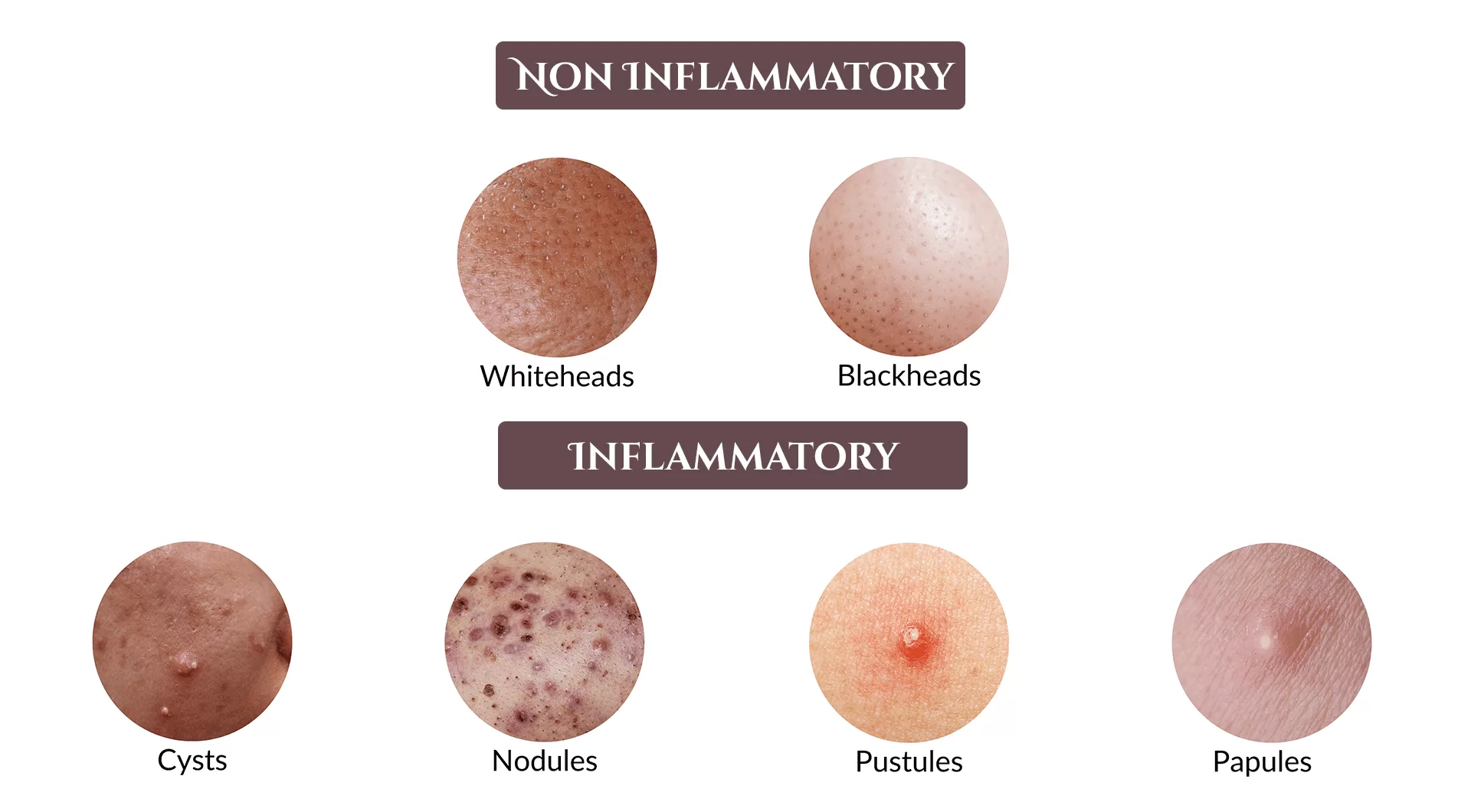
What does hormonal acne look like?
Hormonal acne manifests in various forms such as whiteheads, blackheads, papules, pustules, cysts, and nodules. Whiteheads and blackheads typically lack inflammation or swelling, although if these symptoms arise, they often signify the development of cysts and pustules. Cysts, which form beneath the skin’s surface, tend to be tender or painful upon touch. Inflamed acne presents with redness, swelling, soreness, and discomfort.
The distribution of hormonal acne across the body varies depending on age and health. Adolescents commonly experience lesions on the T-zone (forehead, nose, and chin), while adults aged 20 or older typically encounter breakouts on the lower regions of the face, such as the jawline, chin, and lower cheeks. However, hormonal acne can also emerge on the neck, back, shoulders, and chest.
Challenges and characteristics of hormonal acne
Hormonal acne may not always respond completely to traditional acne treatments like topical retinoids and antibiotics. Even Isotretinoin (Isotretinoin/Accutane) may not yield satisfactory results in some cases, and there’s a higher likelihood of hormonal acne recurrence following successful treatment with Roaccutane (Accutane).
In addition to being resistant to treatment, hormonal acne can lead to prolonged redness, scarring, and pigmentation issues. Certain types of hormonal acne, particularly those affecting the temples, cheeks, and jawline, may result in numerous comedones.
Enlarged pores on the nose and cheeks are commonly associated with hormonal acne, contributing to frustration and a diminished quality of life for those affected.
Hormonal acne differs from fungal acne based on the appearance and location of the lesions. Fungal acne typically presents as smaller, evenly sized spots.
Can hormonal acne cause scarring?
Hormonal acne can result in scarring, particularly when the acne is severe and inflammatory. Deep inflammation from hormonal acne can damage the surrounding tissue, leading to scars. These scars may appear as depressed areas (atrophic scars) or raised, thickened areas (hypertrophic scars). Seeking appropriate treatment for hormonal acne is crucial to minimize the risk of scarring and effectively address any existing scars.
While hormonal acne typically doesn’t cause scarring as frequently as teenage acne, it can still occur, especially if blemishes are manipulated. Therefore, it’s important not to attempt to “pop” any blemishes at home to prevent scarring.
How do I prevent acne?
Preventing acne and minimizing the risk of scarring involves a combination of skincare practices, lifestyle changes, and avoiding certain triggers.
Tips to help prevent acne and minimize the risk of scarring
Here are some tips to help prevent acne and minimize the risk of scarring:
Keep your skin clean
Wash your face twice daily with a gentle cleanser to remove dirt, oil, and impurities that can clog pores and lead to acne. Avoid harsh scrubbing, as this can irritate the skin and worsen acne.
Use non-comedogenic skincare products
Choose skincare and makeup products labeled as “non-comedogenic,” meaning they are less likely to clog pores and contribute to acne formation.
Moisturize
Use a lightweight, oil-free moisturizer to keep your skin hydrated without clogging pores. Moisturizing can help maintain the skin barrier and prevent excessive dryness, which can trigger acne.
Avoid touching your face
Touching your face can transfer dirt, bacteria, and oils from your hands to your skin, leading to breakouts. Avoid touching your face unnecessarily, and wash your hands frequently, especially before applying skincare products or makeup.
Limit sun exposure
While moderate sun exposure can have benefits for acne-prone skin, excessive sun exposure can worsen acne and increase the risk of scarring. Use sunscreen daily, preferably with a non-comedogenic formula, and wear protective clothing and hats when spending time outdoors.
Manage stress
Stress can exacerbate acne by triggering hormonal changes that increase oil production and inflammation. Practice stress-reduction techniques such as mindfulness, meditation, yoga, or deep breathing exercises to help manage stress levels.
Avoid picking or popping pimples
Picking or popping pimples can worsen inflammation, increase the risk of infection, and lead to scarring. Instead, allow acne lesions to heal naturally or seek professional treatment from a dermatologist.
Maintain a healthy diet
While diet alone may not directly cause acne, certain foods and dietary habits can contribute to acne flare-ups in some individuals. Limit consumption of high-glycemic foods, dairy products, and foods high in saturated fats, and focus on a balanced diet rich in fruits, vegetables, whole grains, and lean proteins.
Stay hydrated
Drink plenty of water to keep your skin hydrated and promote overall skin health. Adequate hydration can help maintain skin elasticity and reduce the risk of scarring.
Avoid irritating ingredients
Some skincare products and ingredients can irritate the skin and exacerbate acne. Avoid products containing alcohol, fragrances, and harsh chemicals, and opt for gentle, non-irritating formulations instead.
By incorporating these preventive measures into your skincare routine and lifestyle, you can help reduce the likelihood of acne breakouts, minimize inflammation, and lower the risk of scarring. If you continue to experience persistent or severe acne, consult Direct Aesthetics for personalized treatment recommendations.
How to treat hormonal acne
Here’s the scoop: You’re not stuck with those pesky cystic breakouts forever. Acne, including hormonal acne, typically gets better as your body adapts to hormonal shifts or other changes.
It’s totally normal to experience breakouts, and luckily, there are plenty of treatment options available to help manage them. However, be cautious of so-called “natural” remedies you might find online, like certain essential oils—they’re not always reliable and could even aggravate the situation. At Direct Aesthetics, we suggest exploring the hormonal acne treatments listed below instead.
Microneedling
Microneedling addresses a range of skin concerns, including fine lines, wrinkles, stretch marks, sagging skin, and scarring. It’s particularly effective in reducing acne scars and enhancing the texture of crepey skin. Even in delicate areas like around the eyes and mouth, microneedling proves effective in reducing wrinkles, imparting a rejuvenated appearance to the complexion.
By creating tiny channels in the skin, microneedling enhances the absorption of skincare ingredients applied post-treatment, such as hydrating hyaluronic acid. Studies have shown a significant increase in collagen and elastin production in the skin following just one microneedling session, leading to improved skin texture and resilience.
Is microneedling good for acne breakouts?
Using microneedling on active acne lesions can exacerbate the condition.
Pustules, pimples, inflammation, nodules, or any form of active breakout should be completely avoided. Microneedling can inadvertently spread acne bacteria beneath the skin’s surface, potentially triggering more severe flare-ups.
The same caution applies to skin experiencing active eczema, psoriasis, or any other form of irritation.
Preferable options for managing acne
It’s advisable to address acne before considering microneedling. This can typically be achieved using topical products like BHAs, benzoyl peroxide, tretinoin, or professional skin treatments such as chemical peels. The choice of treatment depends on the underlying causes and severity of the acne.
Chemical Peels for Acne
You might be familiar with the idea that chemical peels can enhance your skin’s appearance overall, but did you know they’re also commonly used for treating acne? Acne doesn’t discriminate based on age or life stage. It can affect teenagers preparing for a school event, adults dealing with post-pregnancy breakouts, or even older individuals experiencing hormonal shifts, medication effects, or stress-related flare-ups.
VI Peel
For individuals grappling with acne, the VI Peel is a promising treatment option that serves as an alternative to oral medication. The VI Peel treatment targets acne scars, pigmentation, and signs of aging by exfoliating the skin’s surface. It mitigates inflammation, clears congested pores, and combats acne-causing bacteria. By accelerating the skin’s natural cell turnover process, the VI Peel reveals fresh, healthier skin layers. Learn more about the VI Peel and its benefits.
Over-the-counter cleansers
Consider over-the-counter cleansers containing chemical exfoliants. These ingredients, such as alpha hydroxy acids (AHAs) like glycolic or lactic acid, beta hydroxy acids (BHAs) like salicylic acid, and benzoyl peroxide, help loosen the bonds between dead skin cells, preventing pore-clogging buildup. Tammy Kirby, DNP, suggests exploring different options to find what works best for you.
SkinBetter Science Cleansing Gel
SkinBetter Science’s Cleansing Gel is designed to provide a gentle yet effective cleansing experience, suitable for all skin types, including acne-prone skin.
Here’s how SkinBetter Science’s Cleansing Gel can help:
- Thorough Cleansing
The Cleansing Gel effectively removes impurities, excess oil, and makeup from the skin’s surface, helping to prevent pore congestion and breakouts. Proper cleansing is essential for maintaining clear and healthy-looking skin, especially for individuals prone to acne. - Non-Stripping Formula
Unlike harsh cleansers that may strip the skin of its natural oils and disrupt the skin barrier, the Cleansing Gel features a gentle, non-drying formula. It cleanses the skin without leaving it feeling tight or irritated, making it suitable for daily use. - Balanced pH
The gel-based formula is formulated with a balanced pH, helping to support the skin’s natural acid mantle. This pH balance is crucial for maintaining optimal skin health and preventing excessive dryness or oiliness, which can contribute to acne development. - Refreshing Sensation
The Cleansing Gel provides a refreshing sensation upon application, leaving the skin feeling clean, refreshed, and revitalized. Its lightweight texture makes it ideal for use in both morning and evening skincare routines. - Prepares Skin for Treatment
By effectively removing surface impurities, the Cleansing Gel prepares the skin to receive the full benefits of subsequent skincare products, such as serums, moisturizers, and acne treatments. Clean skin allows for better product penetration and absorption, maximizing the efficacy of your skincare routine. - Dermatologist-Tested
SkinBetter Science products, including the Cleansing Gel, undergo rigorous testing and are developed with dermatologist input to ensure safety, efficacy, and compatibility with various skin types. This commitment to quality and innovation makes SkinBetter Science a trusted choice for skincare enthusiasts and professionals alike.
Overall, incorporating the SkinBetter Science Cleansing Gel into your daily skincare routine can help promote a clear, balanced complexion while providing a refreshing and enjoyable cleansing experience. As with any skincare product, it’s essential to patch-test before regular use and discontinue use if any irritation occurs.
Topical retinoids
SkinBetter Science offers a range of products that may benefit individuals with acne-prone skin by addressing concerns such as oiliness, congestion, and inflammation. Here are a few Skinbetter Science products that may be beneficial for acne-prone skin:
AlphaRet Clearing Serum
Skinbetter Science’s AlphaRet Clearing Serum is formulated to address acne-prone skin by combining the benefits of retinoid and alpha hydroxy acid (AHA) technology.
Here’s how AlphaRet Clearing Serum can help:
- Retinoid Benefits: Retinoids, derived from vitamin A, are known for their ability to promote skin cell turnover and unclog pores. By accelerating the shedding of dead skin cells, retinoids help prevent the formation of comedones (blackheads and whiteheads) and reduce the likelihood of acne breakouts.
- AHA Exfoliation: The serum contains alpha hydroxy acids (AHAs), such as glycolic acid, which provide additional exfoliation benefits. AHAs help to further remove dead skin cells from the surface of the skin, improving skin texture and minimizing the appearance of acne scars and hyperpigmentation.
- Clarifying and Brightening: Along with its acne-fighting properties, the AlphaRet Clearing Serum also works to clarify and brighten the complexion. By promoting cell turnover and exfoliation, it helps reveal smoother, more radiant skin.
- Targeted Treatment: The serum is designed to target multiple aspects of acne-prone skin, including clogged pores, excess oil production, and uneven skin tone. Its comprehensive approach makes it suitable for individuals looking to address both active breakouts and residual acne marks.
- Consultation: Before incorporating any new skincare product into your routine, especially one containing active ingredients like retinoids and AHAs, it’s advisable to consult with a skincare professional such as Direct Aesthetics. They can assess your skin’s specific needs, provide personalized recommendations, and guide you on how to integrate the product effectively and safely into your skincare regimen.
If you’re considering using the AlphaRet Clearing Serum, it’s essential to follow the recommended usage instructions and gradually introduce it into your routine to minimize the risk of irritation or sensitivity.